
Professor Paul Cosford is director for health protection and medical director at Public Health England, an executive agency of the UK Department of Health (DoH) established in 2013.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
He is responsible for the national delivery of services to prevent and control infectious diseases and environmental hazards, and for public health emergency preparedness and response.
Cosford has led the national and local delivery of health protection services within the Health Protection Agency since September 2010, and acted as chief executive of the organisation from October 2012 to February 2013. Previously, he was the regional director of public health for the East of England, leading strategies for health inequalities and health improvement, the health system’s response to pandemic flu, and the reduction of healthcare associated infections.
Julian Turner: Please describe Ebola screening procedures at UK airports including Heathrow.
Paul Cosford: Passenger data is used to identify those passengers who have recently travelled from Liberia, Sierra Leone and Guinea on routes with onward connection to the UK.
Passengers have their temperature taken and complete a questionnaire asking about their current health, their recent travel history and whether or not they might be at potential risk through contact with Ebola patients.
Based on the information provided and their temperature, passengers will be given advice and allowed to continue on their journey, or undergo a clinical assessment by Public Health England (PHE) staff – and if necessary be transferred to hospital for further tests.
JT: If passengers flying from international airports in affected West African countries are already being screened for Ebola prior to take off, is entry screening in the UK really necessary?
PC: Although no system can completely prevent a case of Ebola coming into the UK, enhanced screening in high-volume ports of entry will ensure that individuals at risk know exactly what to do if they start feeling ill, and can immediately receive the expert advice that they need.
JT: Is PHE confident that robust exit screening procedures are in place at airports in West Africa?
PC: PHE is working with the international community and local health authorities to ensure robust exit screening remains in place at airports in Sierra Leone, Guinea and Liberia, which will pick up anyone who is symptomatic before they leave these countries.
JT: What lessons have been learned from the 2003 SARs outbreak in terms of passenger screening at airports and do UK authorities plan to introduce technology such as thermal scanning?
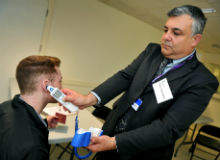
PC: PHE uses an accurate, clinically validated, tympanic (ear canal) thermometer – a standard instrument in widespread use throughout the UK National Health Service (NHS) – combined with a technique that does not involve the screening staff having direct personal physical contact with the person being screened.
The thermometer has a new disposable hygiene shield fitted to the thermometer head for use on each individual person being examined to ensure good infection control between the passengers being screened, and between them and the person performing the screening procedure.
If we were to refer a person to secondary care for assessment because of an elevated temperature, then the first test that would be done would be to measure that person’s temperature with a clinically validated tympanic thermometer.
On that basis, it makes sense for us to use the most accurate thermometer that we have at our disposal during screening, one that is compatible with or identical to the type of thermometer that is in use in the NHS for formal clinical assessment.
JT: Does airport entry screening go far enough when you consider that Craig Spencer and Thomas Eric Duncan weren’t identified as having Ebola when they returned to the US earlier this year?
PC: The opportunity to undertake medical assessment by trained medical personnel at these busy ports builds on the standard protocol for all UK airports where an assessment is undertaken if someone arrives displaying symptoms of any serious illness.
It is important to remember that, overall, the risk of Ebola in the UK remains low, and that we have a world-class domestic health system that is ready to respond if we do witness a case in the UK.
JT: Is it true that screening travellers when they land only identifies those who develop symptoms during the flight, which is unlikely given that the Ebola incubation time is on average nine days?
PC: We have always been clear that no system can completely prevent a case of Ebola coming into the UK, but enhanced screening will ensure that individuals at risk know exactly what to do if they start feeling ill and can get in touch with the expert advice they need immediately.
JT: Have UK airports had to employ additional staff to carry out Ebola screening and are there any new detection technologies or procedures that PHE plans to introduce?
PC: PHE employees plus staff from the civil service are delivering the enhanced screening in selected UK airports and ports. At each airport and port where screening is being undertaken, each shift always includes appropriate health protection practitioners to oversee any clinical assessment required. These are all PHE employees and are largely nursing staff.
PHE is continuously reviewing the screening programme and has made a number of improvements to practice since it was first introduced. We have, of course, also looked at practices again in the light of the recent UK case of Ebola to see what lessons can be learned. Further guidance, in line with existing practice and algorithms, has been issued to staff undertaking risk assessments.
JT: How do you respond to criticism of Ebola screening procedures in light of the recent case involving Scottish nurse Pauline Cafferkey?
PC: The patient was on the returning worker scheme and was screened at Heathrow Airport on arrival, in line with standard procedures. At this point, Ms Cafferkey did not have any symptoms of a fever, and also stated that she had been well in the previous 24 hours and was cleared to travel home as per the protocol. This process was overseen by a medical consultant.





